Tag: child Ortho

As part of #CerebralPalsy Awareness day that just passed us we are organising a two day programme for children with #PediatricOrthopedic Disorders, #CerebralPalsy, #NeurologicalDisorders, #Autism .
The programme is slated to be held for 2 days April5th and 6th.
Timing is between 8 30am and 1pm.
Prior registration is mandatory. This can be done by calling +919495888879.
The first day April 5th Friday for Pediatric Neurological disorders like seizures, autism and second day on April 6th Saturday. The event would be marked by free medical examinations camps, art competitions for children, vocational training for mothers abs awareness programme of respective disorders. It is to be held at #Palakkad #Kerala on these two days.
The event is kindly organised by the selfless efforts of people at #Sevabharathi #Palakkad ably guided by Dr. Sreeram Sankar , Biju Bhasker of #LifeCarePhysiotherapyCentre, Palakkad and assisted by Vinod Kumar of NationalOrthotics, #Coimbatore and several other sponsors. Dr. Velmurugan , Pediatric Neurologist would be part of the event on April 5th and Easwar Tr Pediatric Orthopedic Surgeon will take part on April 6th.
Please share the news !
Thank You
Dr. Easwar TR

Recently gave an interview to a popular news channel in #Kerala in #Malayalam.
The topic was “Common Children’s Orthopedic Disorders and Cerebral Palsy”.
It’s is in an interview format with patients who are interested phoning in the channel to discuss some of their doubts about these disease conditions.
The idea was to take up and discuss the most common children’s bone diseases that parents would need guidance on like Bow Legs, Knock Knees, Club Foot, TB infection of Bones, Perthes Disease of hip, Cerebral Palsy and interact with patients who may phone in.
Common Bone and Joint Problems in Children and Cerebral Palsy
(This interview would be in the local language of Kerala State, Malayalam )
Dear Friends ,
I have great pleasure to announce that along with the launch of a Cerebral Palsy Clinic at Sri Ramakrishna Ashrama Charitable Hospital , Thiruvananthapuram, Kerala I am also starting an exclusive Pediatric Orthopedic Clinic.
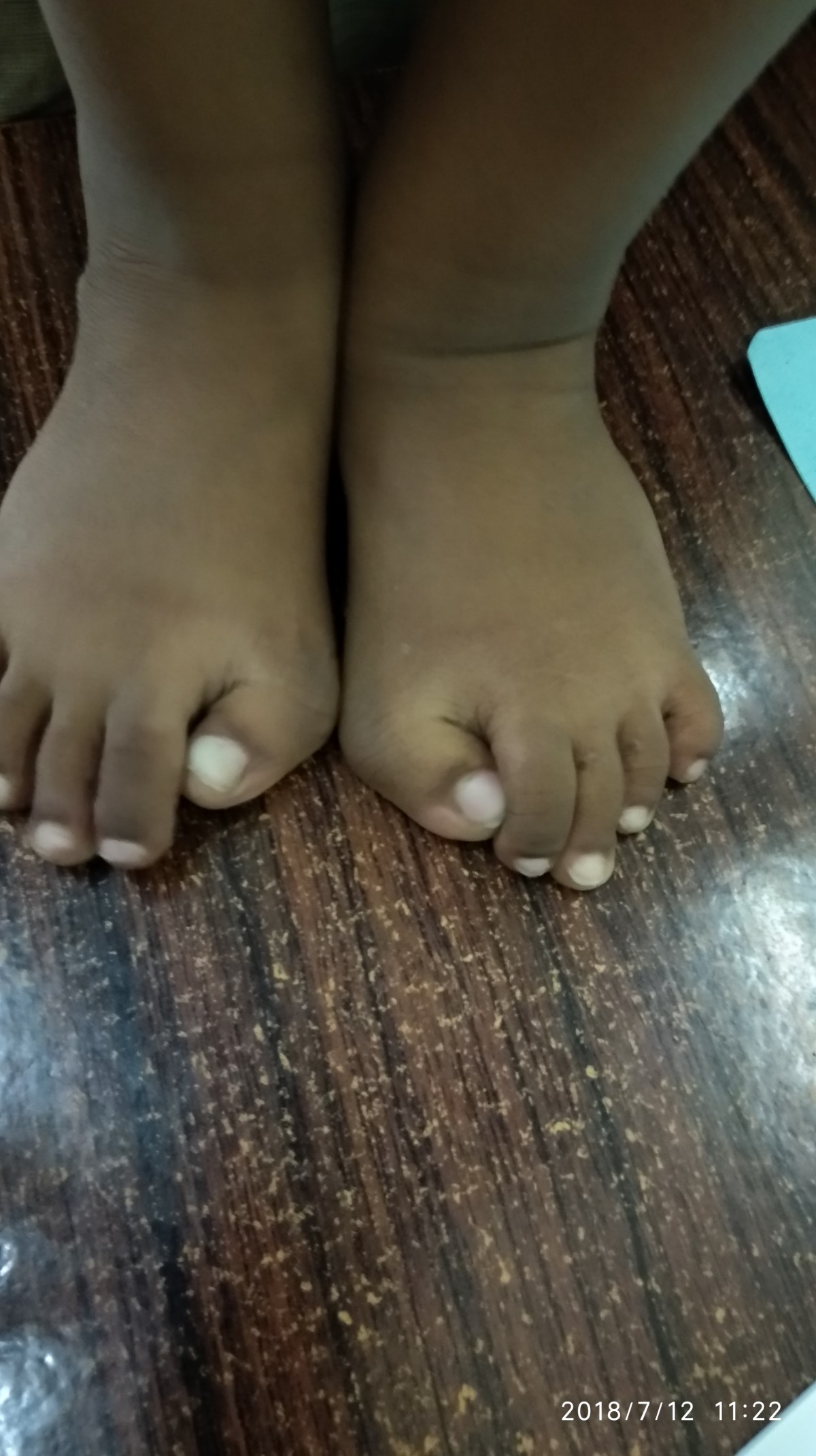
This will cater to children suffering with bone and joint disorders, congenital deformities like Club Foot, Flat foot, Knock Knees and Bow legs among many others. Treatment advise for Spine problems in children like spina bifida, congenital and idiopathic scoliosis are also offered.
I am hereby attaching a video clip showing the many clinical conditions for which services are being offered here.
This hospital being a charitable one caters to the poor and these services would be of benefit to many.
Kindly share among your friends so that people are aware of the new service.
Dr. Easwar TR
Pediatric Orthopedic & Spine Surgeon

Delighted to announce an Art Project with Dr. Suresh (Director , Neurologist , ICCONS) , Dr. Sekar Michael ( Pediatric Anesthetist, ICCONS) and Dr. Easwar TR (Pediatric Orthopedic & Spine Surgeon , ICCONS) as fund raising campaign for treatment of children with #CerebralPalsy, Movement Disorders, Chronic Pain and #Autism. This will be an ongoing project.
First day was today. Wonderful experience at ICCONS, Shoranur.
Lovely to see that many of the staff from Speech and Audiology participated as well.
We plan to improve this in the next iteration and pool all the paintings we paint ( Dr. Suresh, Dr. Sekar and myself ) to help build a fundraiser.
We will be holding these painting sprints at frequent intervals.

#


















ArtForACause
#Art
#Painting

DDH otherwise called Developmental Dysplasia of Hip is a condition where the ‘ball-and-socket-joint’ of the hip is not formed well at birth. It used to be called Congenital Dislocation of Hip.
The child is born with a slightly misfitting hip joint where the ball is slightly shifted out of cup or a hip joint where the ball is completely outside the cup and cup is also very shallow. This can occur on one side or both sides.
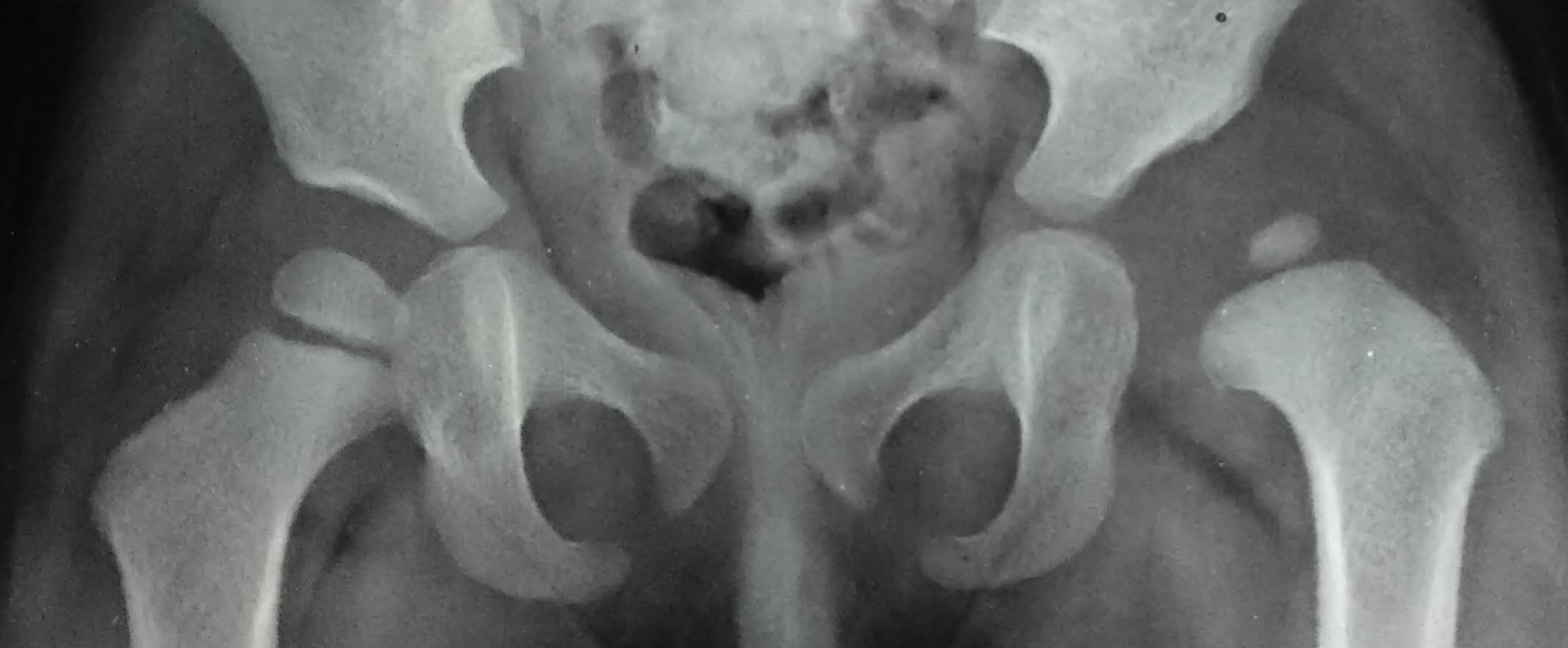
Why does it happen ?
Most times its ‘Idiopathic’ , a medical term which means – cause is not known. In many other patients, the child will be having one of the syndromes (a group of clinical features and disorders in other organs systems and external appearance) or neurological issues in the spine (like meningomyelocele) that also causes this. This second group is sometimes medically referred to as Teratogenic DDH and is much more difficult to treat.
We will discuss below the aspects as related to Idiopathic DDH. They don’t apply to Teratogenic or Neurological DDH.
How do we know the child has DDH ?
Most newborn screening procedures at the hospitals have doctors checking to see if the new born child has clinical signs of DDH. It is easiest to detect and treat it at that early stage.
Once a clinical suspicion of DDH is there the Neonatologist usually refers the child to a Pediatric Orthopedic Surgeon. In addition to establishing the clinical diagnosis by physical examination, the doctor will order an x-ray and an Ultrasound Scan of the Hips to check the dislocated hips. Several measurements need to be taken and ease of dislocation need to be established under Ultrasound scan by a procedure called Dynamic -Ultrasound. The treatment starts after these are done.
In many children, the initial diagnosis may not be made in the immediate post-delivery period. Children may be brought to the OPD by parents with complaints that the thigh skin fold dont look symmetrical and the hips don’t open out fully for parents to change diapers.
In older children parents may notice a limp when the child walks or a limb length difference may also be noted with the dislocated side being shorter.
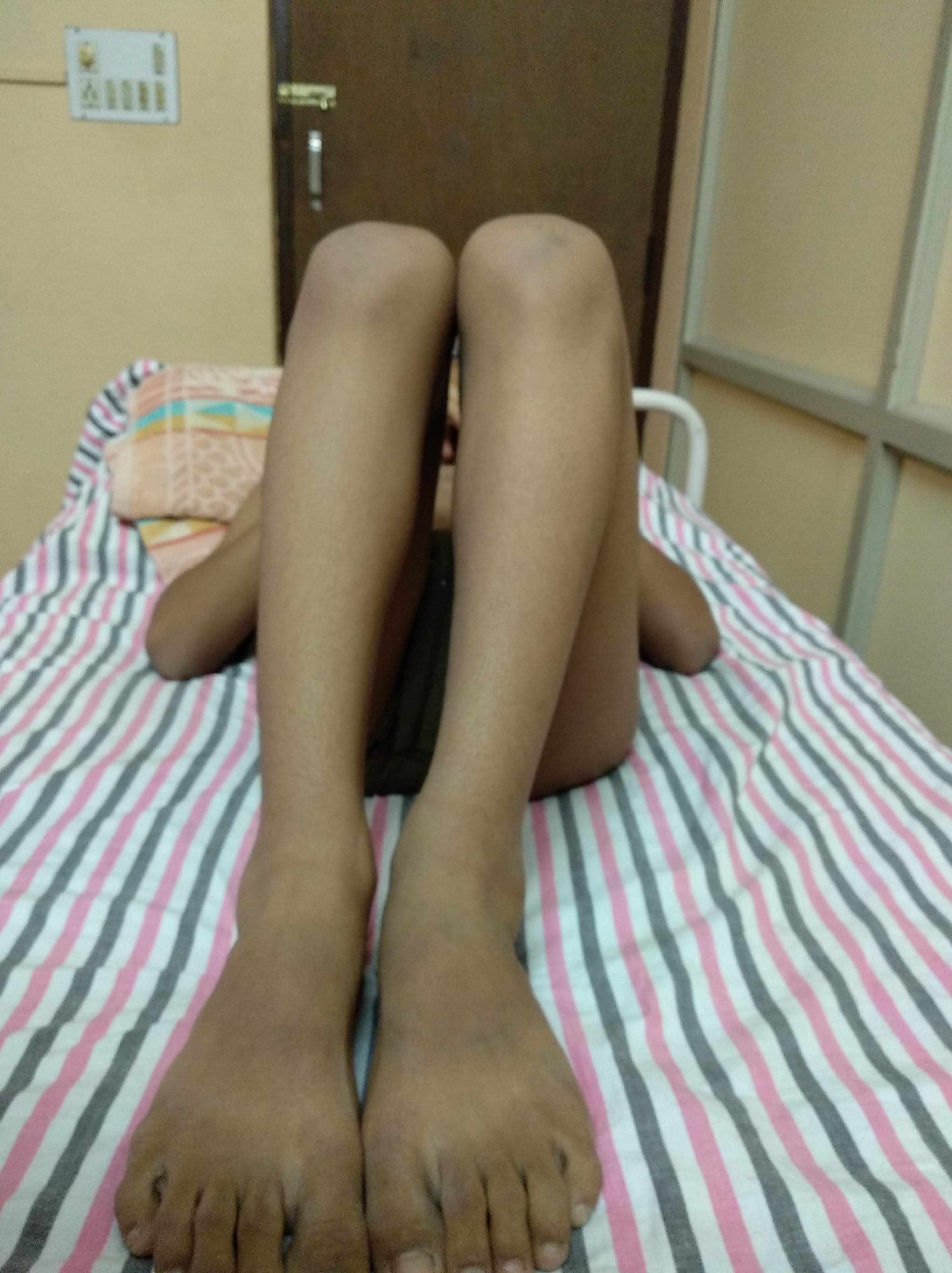
How soon should the treatment start ?
As described in previous section, treatment should ideally start in neonatal period once the problem has been detected. After clinical examination and Ultrasound examination, your doctor will suggest usually a belt type device called Pavlik Harness to be applied on the child to keep the hip reduced inside the cup. This harness is to be worn full time. Parents are counselled on how this is applied and how the straps are tightened.
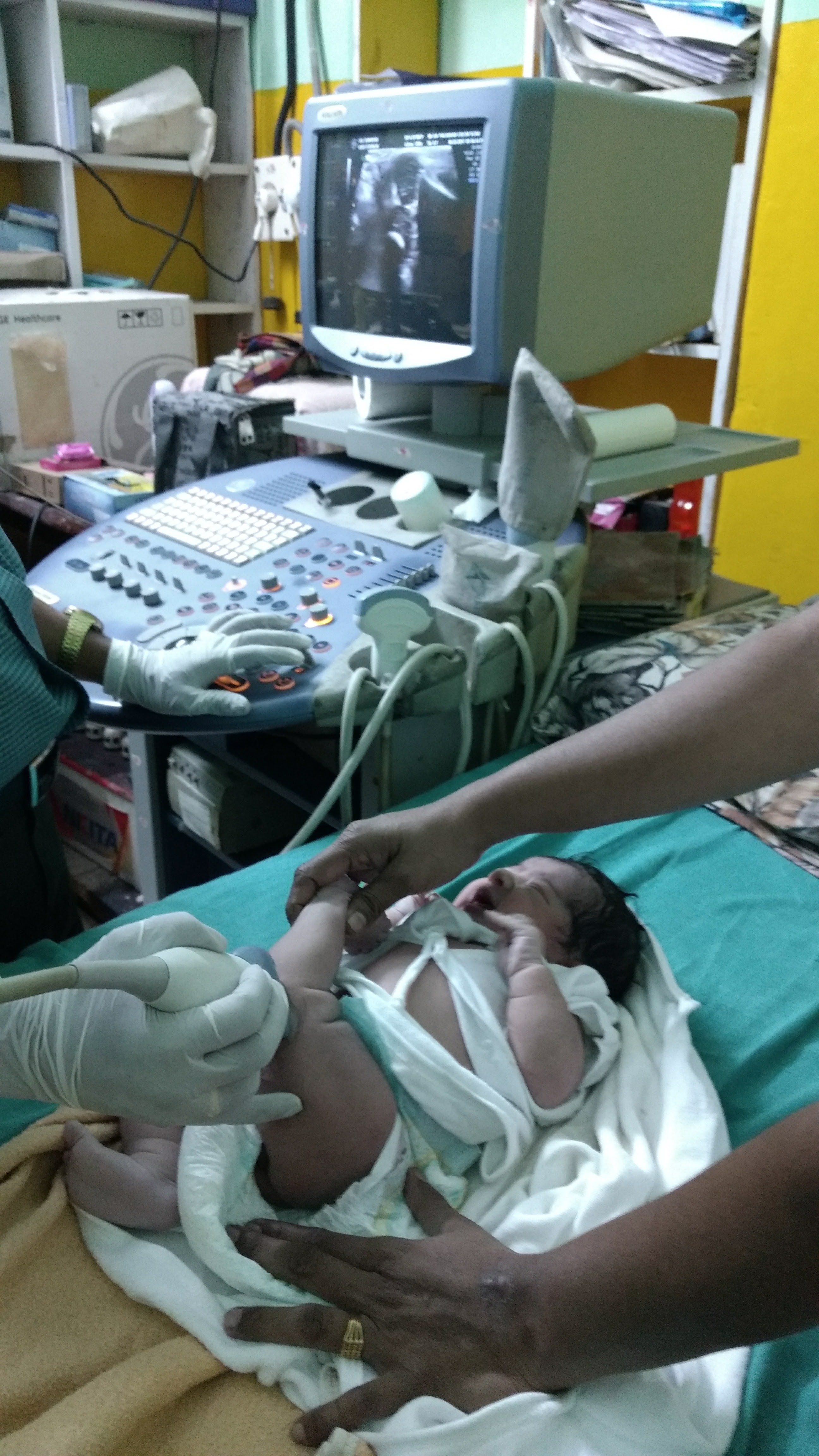
Once this harness has been applied, the hips are scanned with Ultrasound every 2 weeks to check for improvements. Ideally this has to be kept for about 3 months and taken off after the hip stabilizes inside the socket. A slow weaning period is there before the child can be fully taken off the Pavlik Harness. This is to ensure that the Ball ( head of femur ) stabilizes inside the socket (Acetabulum of Pelvis) and the hip is stable. The tissues around the hip also has to shrink and adapt to the new location of Head of Femur. Otherwise re-dislocation or partial slip (medically called subluxation) is a possibility.
In many cases the parents may not be willing for a device to be applied on the child full time post-delivery or the DDH itself may go undetected. This child eventually may be brought later in life by the parents with complaints necessitating surgical procedures.
What is the treatment options for DDH?
As previously described if the newborn is detected to have DDH the treatment is to apply Pavlik harness on the child after Ultrasound exam proves hip is reducible and stable in what is called a safe zone. Safe Zone is a zone where the position in which the harness has to be applied to the child does not compromise the blood supply the head of femur. This is very important decision to make.

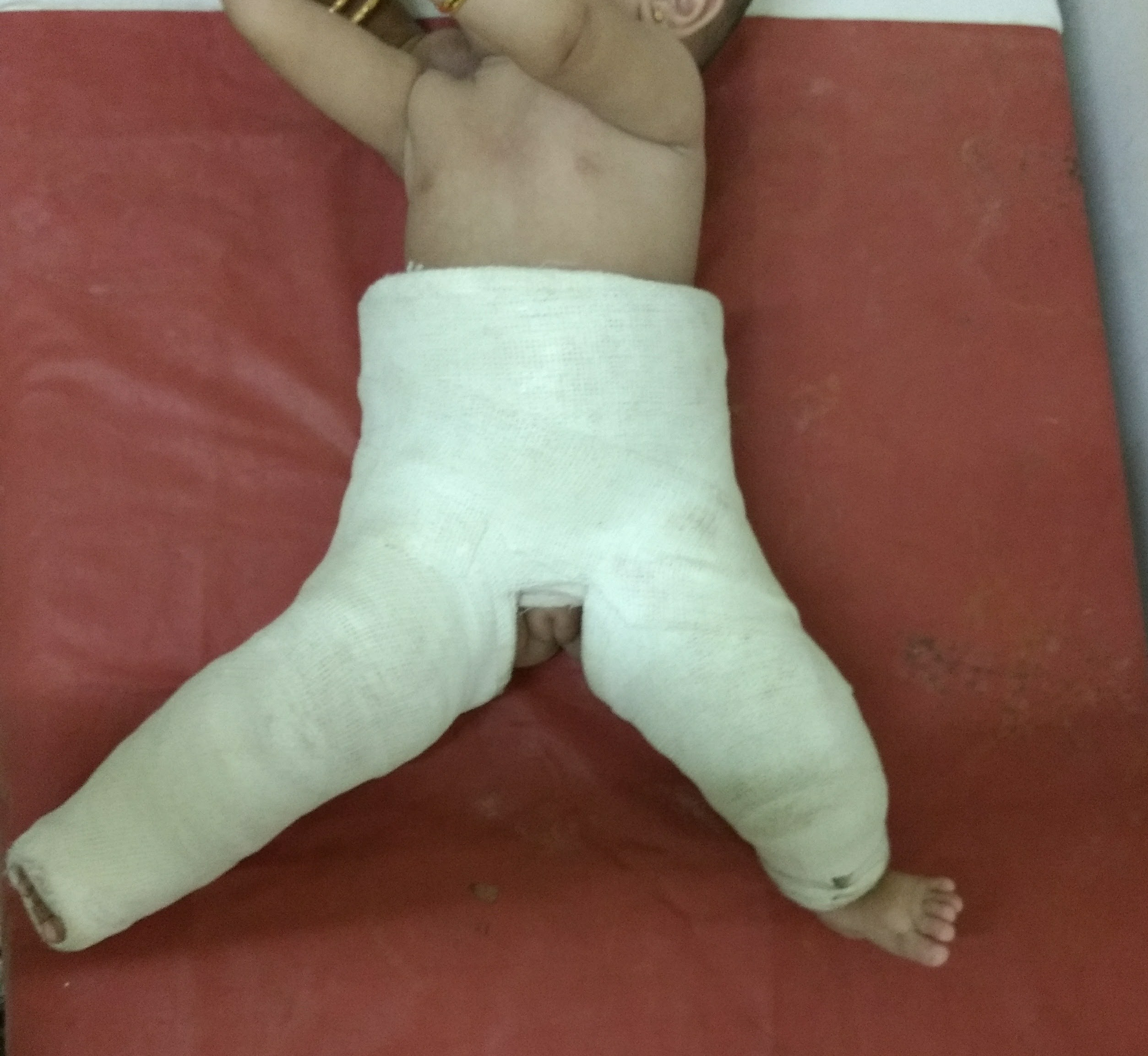
If the child is brought later in life, before 1 year, the hip has to be checked for reducibility as the tissues around the hip would have become contracted and sometimes it is difficult to reduce the hip back into the socket. Usually anaesthesia would be required and the hip once reduced back into the socket is held there by application of the plaster of paris or POP called Hip Spica. This is kept for approximately 3 months until the hip has stabilised inside. A CT scan to verify whether the hip is reduced should be done while child is in POP as slippage of the hip socket is also seen when POP cast becomes loose with time.
Surgery is the only option in older children with DDH. These range from relatively simple procedures to complex hip reconstruction procedures depending on age of the child, slope of cup, angle of rotation of the neck of the thigh bone and shape of the head. These are best evaluated as per the needs of the child.
Generally these surgical procedures can be grouped into a few types :
- Open Reduction of Hip and Capsulorraphy (medical term meaning stitching up of capsule or the covering around the joint)
- This is basic necessity. Here the hip is reduced back into the socket and the covering, the capsule, which is loose is tightened with several sutures
- Femur Derotation Osteotomy with shortening
- This would involve a slight shortening of the hip bone and turning it around. The bone would then be stabilied with a metal plate and screws
- The need for your child to have this done depends on the age of the child and the angle of the ‘neck of the femur’, something medically known as Anteversion. This procedure essentially de-rotates the femur neck and allows the head of femur (the Ball) to deeply sit inside the Acetabulum (the socket). A slight shortening of the thigh bone may be needed as the child , if old enough, would have developed tightness of the tissues and hip should be sitting inside the socket slightly loose than in tension.
- Acetabular Osteotomy
- In many children, when they present to the clinic their Acetabulum would be shallow and not deep enough to receive the Head of Femur. In such children deepening of the Acetabulum by a surgical procedure called Osteotomy (a type called Salter Osteotomy being the most popular) may be done.
The above procedures may be combined along with Open Reduction as the surgeon sees fit after evaulating the child. These options and its pros-and-cons would be discussed with the parents before the surgery.
What happens if we don’t treat DDH promptly ?
Best time to treat the child is in the newborn period. With time the tissues around the hip gets tighter and the bone structure of thigh bone and pelvis alters since the normal growth with moulding of the ball being inside the cup doesn’t happen.
This lack of moulding results in a shallow cup. Additionally the thigh bone’s upper end would be twisted out of shape and the ball also would be misshapen since it has not been moulded by the acetabulum.
All these result in a much more complex procedure to try and restore the hip.
Left untreated DDH causes osteoarthritis or the Hip joint and Hip pain in early adulthood often requiring complex reconstructive procedures.
It is best if the treatment is not postponed and done at the earliest.
Hip Dysplasia Awareness Month – June !!
The Hip Dysplasia Awareness Month of June is to educate parents on Hip Dysplasia and its treatment methods. We hope that parents would bring children to care centers at the earliest if suspicion of hip dysplasia is there.
For more information please visit : http://livingwithhipdysplasia.com/june/ or consult your Pediatric Orthopedic Surgeon.
#Torticollis or #WryNeck is a common complaint in #children.
Children will keep neck turned and/or tilted to one side. This can be a sudden occurrence especially after sore throat or upper airway infection, fall or maybe seen after difficult birth due to stretching and injury to the neck muscle (called Sternocleidomastoid .
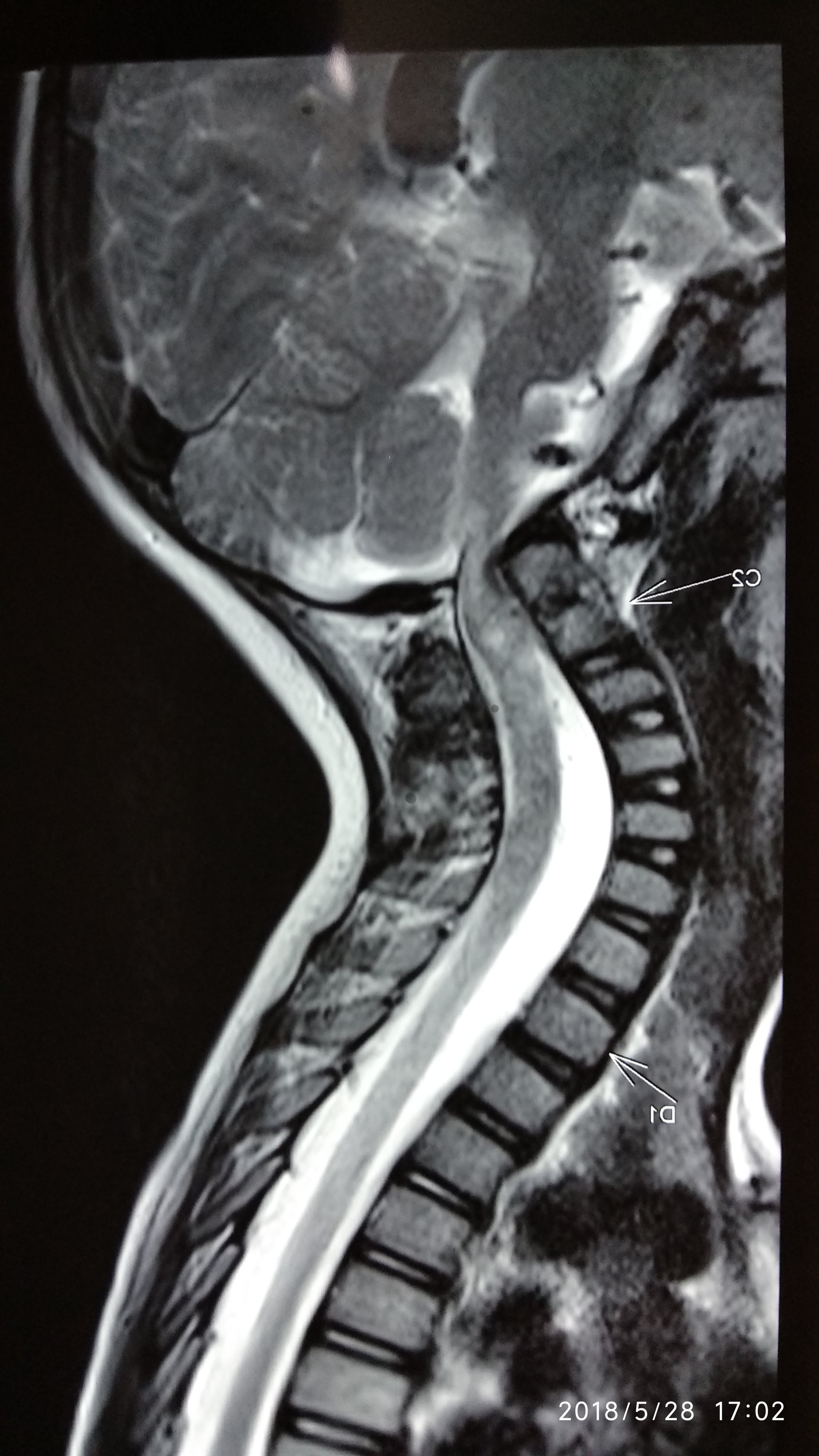
While many are simple spam or contracture of neck muscle some torticollis as shown in the picture below could harbour problems like compression of #spinalcord by #neck bones which have gone off alignment. These problems in the structure of neck bones occur at birth and are due to a developmental error in the shape of the neck vertebra.
#ChildOrtho
#NeckPain
#PedOrtho